It’s 8pm and Mr. Anon is wheeled into the Intensive Care Unit (ICU) at a private hospital in Dar es-Salaam. He is unconscious, and isn’t breathing well.
The nurse on duty – Sister Emous, receives Anon and connects him to the oxygen supply immediately. However, it’s only minutes before the alarm on the monitor starts blaring! Then, a breathing tube is threaded down his throat and connected to the ventilator to support his breathing. Anon will now be cared for by a team of nurses who will tend to him 24 hours a day, 7 days a week.
Sister Emous stands over Anon’s head, looks down at him, and takes a deep breath – she knows there is probably an assembly of very worried, very anxious family members praying and hoping just outside the door.
Anon who isn’t conscious and isn’t breathing on his own, is a typical example of the patients received in the ICU on a daily basis. These patients have several of their organs and body systems out of order and not functioning appropriately. What nurses do for these patients is to basically support their body systems to continue functioning automatically, just as in a person who is healthy and normal.
Checkups that save life
Sister Emous must assess Anon and check the pressure in his brain, his heart rate, and temperature. She must also check how his eyes react to light, how he breathes, how long and fast the breaths are. She evaluates how strong his heart rates are, and if that’s sufficient to support his body. She assesses how and what he eats, making sure this is all in order every hour.
Since Anon is unconscious, he will not be able to cough some secretions out of his lungs. This blocks his breathing pathways. The nurse has to remove the secretions to enable him breathe with ease by performing suctioning with a machine.
That isn’t enough yet
Sister Emous will assess whether Anon can move his limbs or not. If he can, how strong the movements are and if he can’t, she must move them for him to avoid complications that may arise from prolonged immobility. The nurse must make sure to change Anon’s position every few hours to avoid any sores and aches.
She looks out for how much he urinates and how often he does that. She keeps an eye on his bowel movements. She will check and make sure his medications are not interfering with each other and that they are given on time. She will give him a sponge bath, wash his mouth, and ensure his back is oiled and massaged and his bed sheets are fresh and crisp so that he is comfortable and clean.
Sister Emous will be required to draw blood for tests and readings. She will accompany and stand by Anon as he gets his imaging scans while attending to all the alarms and the constant beeping of machines as well as keep an eye on his vital sign readings without resting.
She will communicate with his doctors to update them on the patient’s progress, alert them of anything that may need attention. Sister Emous will also communicate with Anon’s physiotherapists, surgeons, radiographers; even to people who clean the area he sleeps in; making sure that she is thinking critically, always on her toes but still relating Anon’s medical condition to his physiological needs.
Becoming an advocate

Sister Emous will meticulously make sure there isn’t a change in Anon’s condition that is missed. She becomes the advocate for Anon. She makes sure he gets the medications he needs to ease his pain and promote rest. Sometimes she will hold his hand as she performs a painful procedure, at other times she may not be able to. There could be more than one alarm blaring; meaning there is something else to attend to. At that moment, she will look at him and worry, what if Anon is actually his own household’s bread earner? The nurse has to think in Anon’s best interests. She took an oath for that.
As that goes on, this same nurse will forget to pee or even drink water. She will hardly be able to catch a break or settle down, let alone sleep all through the night. While she tends to Anon, she must also attend the other two patients assigned to her care, with conditions similar, if not worse than Anon. And she may worry that the lady in the bed next to Anon has little kids to look after, while she remembers that the old man in the opposite bed has grandchildren crying at the waiting lounge.
It’s morning. Not documented, not done
The cycle continues. When it’s finally 8am and Sister Emous has completed charting and documenting every single thing, little or small that she did for Anon and her other patients all night, she will make sure they are all comfortable. Then, she will hand over the patients to another nurse, her colleague, Brother Alfa. Alfa will now take over Sister Emous’ duties plus her worries and make them his own as if he has been handed over a baton.
Sister Emous will go home to her family but she will not be able to stop thinking about Anon. She will shed some silent tears and say a silent prayer. She will struggle with the several ethical dilemmas she faced all through the night and wonder if she really did her best. She will think about Anon’s wife and daughter, and his old mother, she will recall their sad faces that she saw as she passed by them in the waiting lounge. She will get something to eat and get some rest, only to resume her duty another 12 hours later, all over again.
What about the family?
Nurses leave their own worries outside the gates of the hospital. For the 12 hour duration of their shifts in the ICU, they also forget about their own families and risk their own lives in caring for sick patients.
The aim of nursing care in the ICU is to help the patients regain their bodily functions and keep any compromise in the quality of life at minimum. Therefore, patients in the ICU are in need of utmost, diligent care, especially because they have machines, tubes and medications doing the work of their bodies for them.
They have food pipes and breathing tubes going down their throats and noses. They have tubes to help them empty urine out their bladders and they may have additional drains as well as more than one line inside their veins, with several medications on infusion pumps at once.
Nurses understand that family members of a patient who is in the ICU are worried and at times terrified or heartbroken. They understand that the family wishes they could sit with their patient and take care of them. But the reason any patient gets admitted to the ICU is because the care they need is something only a medically trained personnel can provide.
You are not alone, respect is key
When relatives keep coming inside the ICU or keep requesting to come inside because they are concerned or worried or because they wish to see their beloved one, they must remember that there are several other patients admitted there too; who also have relatives equally concerned.
They are urged to bear in mind that the patient needs utmost calm, peace and rest for all those tubes and medications in place to function the way they are meant to. But equally important, if not more, is to remember that patients, especially those in the ICU, are at their most vulnerable state.
They are unable to protect their own dignity and hence maintaining privacy and confidentiality is paramount. Flocking in or overstaying the allowed timings by relatives may compromise these important aspects of care. Additionally, they must remember that the nurses need the space to work and the calm to function. They need utmost cooperation in order to best take care of these patients.
Kind words can heal the soul
Heaven forbid, you ever have a patient admitted to the ICU; remember to follow the rules of visiting timings and any other rule that may be in place. Remember that the patients have been placed there for a reason that you now understand. Also, next time, remember to say an extra word of kindness or a silent prayer for the nurses who take care of your patient!

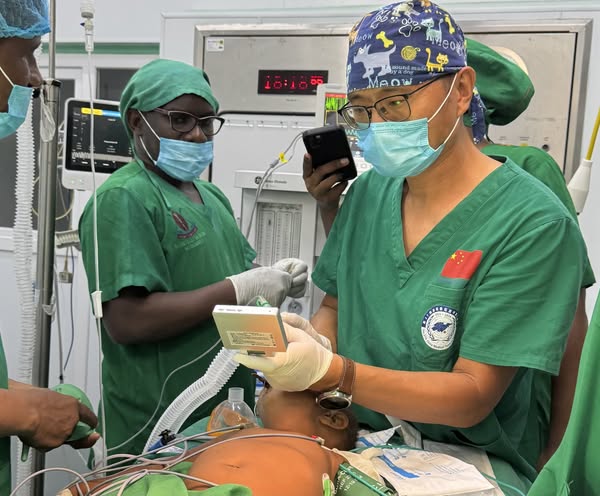
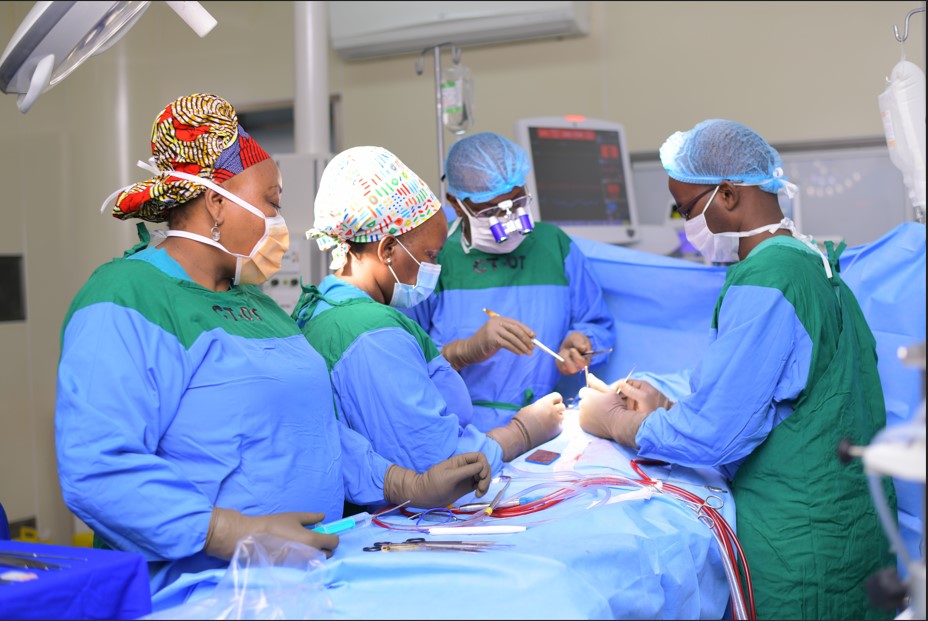





Salute and silent prayers to all the hardworking nurses all over the world.
Amazing insight of your noble profession. Keep it up and may God Bless and protect you and and yours
Appreciate it.
Congratulations my dear, excellent work
Thank you.
BIG UP MY YOUNG SISTER, YOU HAVE DONE A GREAT JOB.
Thank you.
Not documented, not done !!!
number of nurses should increase at leas to reach 3 shifts. this will give enough tome to monitor patients and to document as well.
Indeed Nicolaus. Its a real challenge. Standard needs to be nurse:patient ratio of 1:1 in the critical care setting. Unfortunately it’s almost x3 in reality. And I absolutely agree, not documented, not done.