Three weeks ago, I attended the funeral of my friend’s father. As usual in our setup, before last respects and going to the burial site, we normally have lunch. There was a colourful buffet and a lot of people lined at the table. We were among the last in the line. But in front of me was a pregnant lady, who later I came to understand was among those who had travelled all the way from upcountry, to pay last respects.
Unfortunately, by the time we reached the buffet table, almost all bowls were empty except one with a few pieces of cooked bananas. I could see the frustration on the woman’s face. Angrily as she was, she took those left bananas and went away, quietly. I did not get anything to eat (as well as those who were behind me) but at least I could afford to go to a nearby kiosk to buy something. Not all could do that, including the pregnant woman.
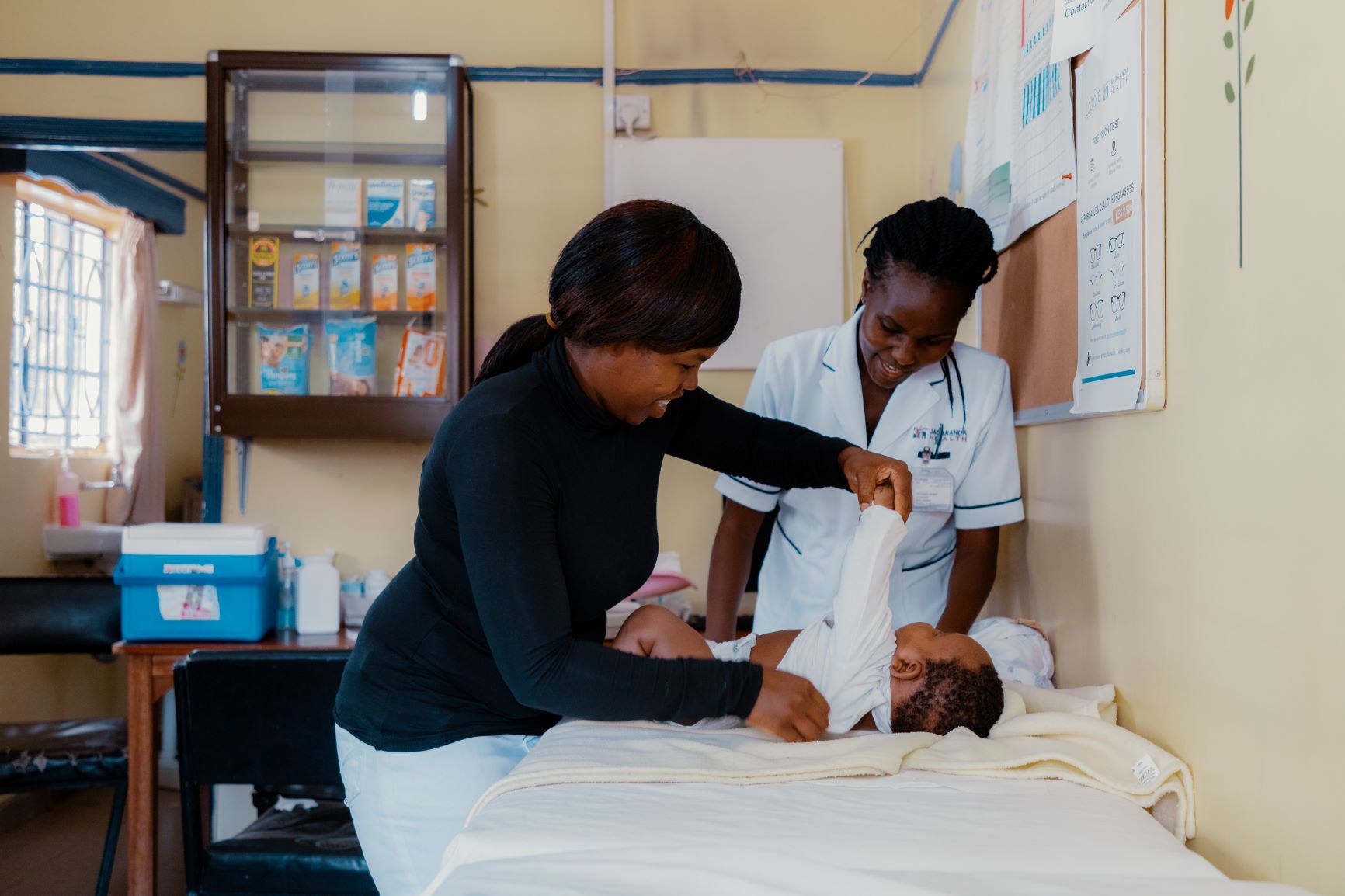
Back in my seat, I was engrossed in thoughts about what had just happened. I started thinking of more or less similar situations happening to our sisters and aunts who attend ante-natal clinics. Often, they attend the clinics to which they are told “it’s free to get services.” However, on reaching the facilities, they usually end up being told “the supplies and drugs are out of stock.”
Those who can afford, can go to a nearby dispensary or drug store while others leave quietly back home, hoping to get the services during the next visit. It’s not just for pregnant women. It also happens to children under five years, the elderly above 60, and the destitute who cannot afford to pay for healthcare.
As we embark on the Universal Health Coverage (UHC) plans, with the slogan ‘No one should be left behind,” it’s important to note that there are groups of people we are more likely to leave behind, if we don’t have carefully planned strategies.
I believe that for successful future strategies on UHC, we have to learn from the past, so that we do not fall again.
Where we’ve come from
Tanzania’s reforms, that aimed to increase access to healthcare, started way back in 1967. The government’s intention was to increase the availability of social services to the poor and those living in the marginalized rural area. During those years, Tanzania became an international reference point in primary health care. And then in 1977 the government banned private for- profit services and privatized all private health facilities.
Another major reform came in the early 90s whereby, due to increased healthcare cost and amid a struggling economy, the government adopted health sector reforms that changed the financing system from tax-based (free care) to mixed financing including cost-sharing. By 1995, cost-sharing was already introduced to all levels of health care provision.
In the early 2000s, an important milestone was reached when Community Health Fund (CHF) and National Health Insurance Fund (NHIF) were introduced; with the former targeting the informal sector and low-income earners.
https://www.youtube.com/watch?v=MjuBH5BoQFE
To date,20 years since the establishment of these funds, less than 15% of Tanzanians have been covered under these arrangements. We should ask ourselves, why? We have to agree, in-country like Tanzania where the tax base is not large enough, a better way to ensure no one is left behind in accessing healthcare is through covering everyone with health insurance. The big question is, why have we not managed to have at least 80% of our people covered?
In my opinion, there are reasons for this:
A: Low government spending on health
For many years, government spending on health has been decreasing. We are far from the World Health Organization’s recommendations of $86 per capita and below the recommended 15%budget allocation as per the Abuja Declaration. It is also known that the 15% is not enough, but reaching the target is a sign of commitment.
In the past 5 years, there has been increased investment health infrastructures, which is a good sign. We hope that this will be supported by an increased investment in human resources, drugs, and supplies as well as quality improvement.
B: Policies and management
This also matters for our colleagues from Zanzibar. The policies that led us to establishing to NHIF and CHF were more inclined towards increasing the source of funds for healthcare, rather than ensuring everyone is covered and can access quality healthcare services. It’s therefore not surprising that policies did not come with a proper way to identify who should be subsidized and how subsidy should be done. Instead, we end up having ‘blanket’ subsidization for ‘special’ groups (pregnant women, under five and elderly) without considering their ability to pay, and even for destitute who were granted with exemption (100% subsidy), no proper definition was set. This has resulted in the limited fund set for the subsidy to benefit more those who can afford to pay than those who cannot. For example, those who can afford to pay a 30,000 CHF premium are subsidized through a matching fund, the same way with NHIF members with a 3% contribution.
In that case, the management of these funds also leaves a lot for improvement, with an example of CHFs which at some point were managed by District Councils with counsellors mandated to set premium to join the scheme. This also created a situation where councils that manage health facilities also managed CHF. This means they were purchasers and providers of services at the same time.
C: Weak Regulation
There are weak regulations in the area of quality of care provision, pricing of services, and insurance benefits issued by private companies. It is difficult for health insurance schemes, especially private ones to survive if there are no regulations on the pricing of health services. We regulate fuel prices due to its importance in the country’s economy. The same should be done for healthcare service prices, as this is important for poverty reduction. Due to poor regulation, currently, there is no minimum benefit package that is allowed to be in the market for health insurance. I have seen insurance packages for only 7 diseases sold in the market. This affects the perception of health insurance in the community and makes it difficult for people in the community to trust health insurance.
D: Public-Private partnership
Since 1977, and after privatization, the relationship between public and private has been weak. This cuts across all areas of service provision; including but not limited to private insurance companies and private healthcare providers (dispensary, clinics, health centers, and hospitals). It is strange that to date, it still looks like a sin for a private health facility to be reimbursed more than a public facility.
E: Community awareness and involvement
It is clear that awareness about health insurance and the importance of risk pooling in the community is still very low. We have not invested enough in this area, which made it difficult for health insurance penetration.
Having looked at where we are, let’s have a look at what can be done:
We need political will.
There are good signs as far as political will is concerned. In the past two elections, all big parties had UHC in the election manifesto. It’s also in the ruling party manifesto. UHC has been highlighted by the Head of State in speeches, and we have seen the intention to table the bill for the UHC.
Inclusive policy for UHC
UHC is not just a health issue. It requires multi-sectoral involvement. According to the World Bank (WB), more than 270,000 people are pushed into poverty everyday due to catastrophic health expenditures. Yet our poverty reduction strategy does not include UHC as one of the strategies to alleviate poverty.
The government’s effort to set aside TZS 400 billion (as per budget speech) to pay for the destitute and those who cannot afford to pay is commended. For this to work, a proper social-economic mapping has to be conducted to identify those who are eligible for the payment. Also, we need to keep this as a reliable source and a sustainable one by amending our tax law to allow for earmarked tax (es) for healthcare. This will mean that money will not be coming at the discretion of a minister or president but rather by law. Ghana has succeeded in this, through 2.5% of VAT and they have managed to cover more than 50% of their population. We have also seen in our country; how successful rural electrification has been, following introducing earmarked tax for the Agency (REA).
Public-private partnership
The involvement of PPP has to cover the whole health financing spectrum, from collection, pooling, strategic purchasing, and payments of providers as well as provision of services. There should be fair rules for both the public and private, and regulations to support the growth of private entities.
Use of technology and data
A lot of things are happening in technology that we could have not imagined 10 years ago. The technology developments and how digital developments have supported revolutions in financial inclusions are known to everyone. It is high time now to tap into these developments to support healthcare access. Technology can be used to identify who needs subsidies and even ensure that entitlements reach the exact person who has been identified so that they can pay for the health care services.
We can also ensure specialized services reach remote areas through telemedicine. There are efforts by the government to distribute digital x-rays facilities to district hospitals, CT-scan to all regional hospitals, and install four radiology interpretation centers to support reading the results from the Regions. This is the way to go! We can use technology to overcome our shortage of trained healthcare workers and also reduce costs of care. With technology, we will be assured of transparency, efficiency, and increased accountability.
To sum up, the WHO estimates that every year more than 5.7 million people died due to poor quality of care. The number of people who are dying due to poor quality of care at health facilities is more than those who are dying due to lack of access to healthcare facilities. If we increase access without fixing the quality challenge, we will be pushing more people to their deathbeds, thinking we are helping them.
This article is an extract of a keynote address during the 8th Tanzania Health Summit, authored by the Country Director of PharmaAccess Foundation Dr Heri Marwa.