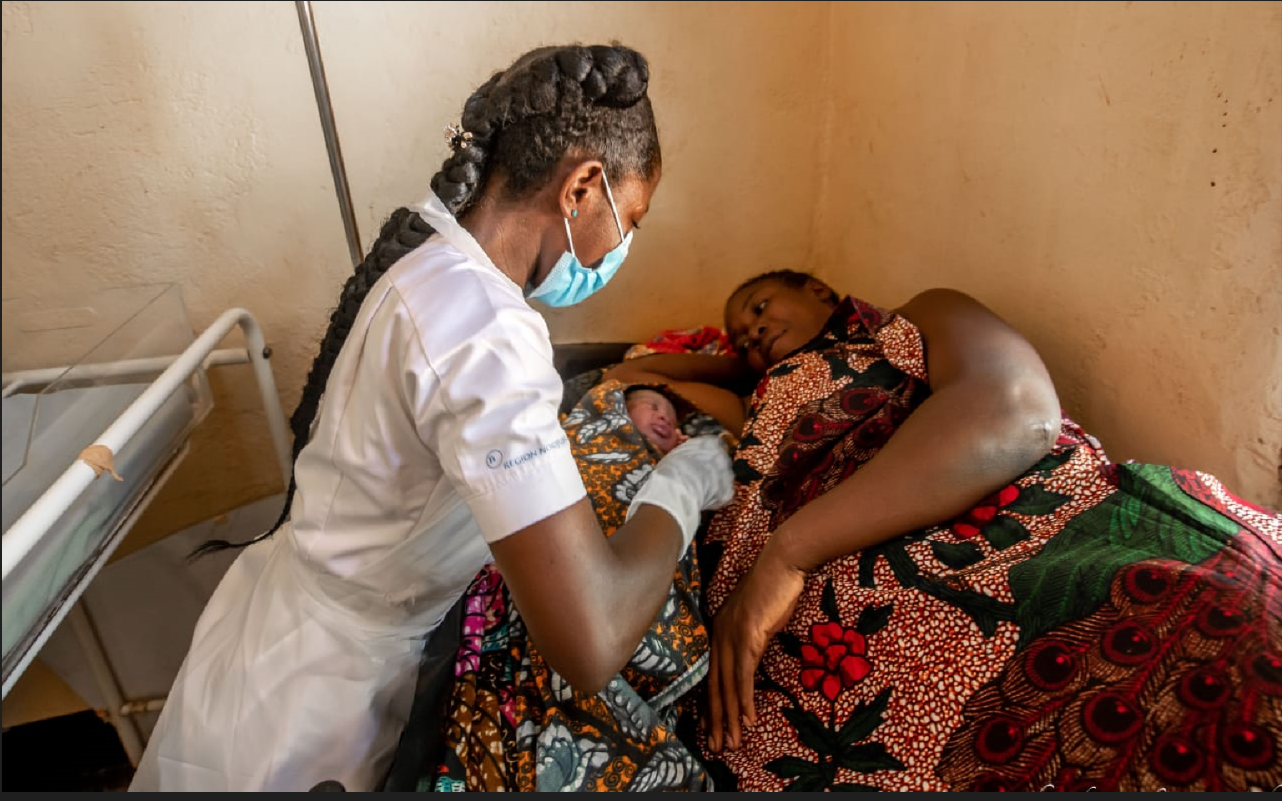
Treasure Nsubuga was 38 weeks pregnant when she noticed that her unborn baby did not seem to be moving as vigorously as it should. Worried that something could have gone wrong, Treasure and her husband went to a local hospital in Kampala, Uganda. On arrival at the hospital, little attention was paid to the mother’s concerns at reception and she ended up waiting four hours to see a doctor. By the time she was seen and referred for an Ultrasound Scan, it was too late. The sonographer could not detect a foetal heartbeat. As a young mother-to-be, she had been excited to welcome her first child into the world. But she had a stillbirth.
“I know for sure we waited for four hours; about four hours and ten minutes,” recalled Treasure. “From that experience I knew that a mother knows and they’re the only voice until a baby comes into the world, so I wished they[at the hospital] would have listened.”
Treasure, a Ugandan, shared her brief story during the International Conference in Maternal and Newborn Health (IMNHC) in Cape Town, South Africa, narrating how she had been treated at a local hospital in her country.
“I just think it was unfair to my baby,” emphasized Treasure, detailing the challenges she faced in accessing respectful and quality maternal and newborn healthcare. She told the conference that despite the government’s policy to provide free healthcare services to mothers and children under the age of five, many families still struggle to receive the care they need.
Tresure’s fears and frustrations are echoed by millions of women and families in many countries, including Tanzania. While there has been progress in increasing coverage of maternal and newborn health services, there is still a critical need to ensure that the quality of care matches the coverage, and that the experiences of healthcare system users are improved.
With a shared goal of advancing the agenda for maternal and newborn health, the stakeholders who gathered in South Africa emphasized the importance of community engagement and social accountability to drive meaningful change.
Reflecting on the challenges faced by mothers like Treasure, they called for the re-envisioning of maternal and newborn health service provision, financing and a paradigm shift towards patient-centered healthcare systems.
Dr. Queen Dube, the co-chair of Align said:”We are even beyond 80% but what is it that is in 80% when a woman comes to deliver at a facility [and] what type of care[is she provided]?”
Dr.Dube and other experts reflected on the progress made towards the Every Newborn Action Plan (ENAP) and the Ending Preventable Maternal Mortality (EPMM) goals, aiming to steer the agenda for maternal and newborn health services forward as a movement, rather than a moment, and creating momentum towards achieving the set targets.
The conference highlighted the significant improvements made in the coverage of maternal and newborn health services in many countries and for Tanzania, with a tremendous increase in the number of CeMONc and BMOC sites. Additionally, the coverage of skilled medical personnel attending to delivering mothers has increased to over 80%, alongside other indicators of coverage, which promises good progress towards achieving the coverage by 2030.
Despite the improvements in the coverage of MNH services in Tanzania like many other countries in Africa, the quality of care remains a critical challenge. While celebrating the increased coverage, the nagging question remains: how do we ensure that the coverage matches the quality of care provided, and how can we improve the experience of healthcare system users?

One of the critical aspects of quality care is respectful maternity care, which poses the urgent need for re-envisioning MNH services financing. While the government has policies in place to provide free healthcare services to maternal services and children under five, the current system does not empower users to demand the quality of care they receive. The perspective needs to shift by ensuring that the power paradigm in healthcare systems turns towards patients (clients) who consume health services. One way to do this is by issuing special health insurance to every pregnant woman and child under five to finance their utilized services.
Coverage versus Quality
While Tanzania has made tremendous progress in increasing the coverage of MNH services, the quality of care provided remains a significant challenge. Despite the government’s policy to provide free healthcare services to maternal services and children under five, the system doesn’t empower users to demand quality care. Health insurance has been proposed as a possible solution, but with over 75% of Tanzanians in the informal sector and most with unpredictable sources of income, health insurance may not be a reliable source of funding for MNH services. Using existing social groups like VICOBA and cooperative unions may help increase enrollment and retention on health insurance schemes.
Respectful Maternity Care
Respectful maternity care is a critical component of the quality of care provided in MNH services. However, it remains a significant challenge in Tanzania. Patients need to be at the center of the health system, and accountability can be set by issuing special health insurance to every pregnant woman and child under five to finance their utilized services. This approach will help shift the paradigm of power in health systems to patients, who consume health services.
Community Engagement
To improve the experience of MNH services, especially in rural areas, community engagement is essential. The Mama Na Mwana (MnM) program is an excellent example of a community social accountability system that enhances community engagement and provides genuine feedback from MNH service consumers. Decision-makers must prioritize community engagement to optimize the use of community social accountability systems to improve the quality of care in MNH services.
Training of Healthcare Workers
Training healthcare workers in customer care is critical to improving the quality of care provided in MNH services. This training should start from training institutions to on-the-job training. Shifting the mindset of healthcare workers from just managing diseases to humanity will significantly improve the user’s experience and ensure quality and respectful MNH services.
Decision-makers must shift the focus of MNH services from coverage to quality and respectful care, more so by re-envisioning of MNH services financing, prioritizing community engagement, and training healthcare workers in customer care. By taking these steps, Tanzania can ensure that all mothers and newborns receive quality and respectful care.