Somewhere in rural Tanzania, a midwife is working alone in a labour ward, with many expectant mothers on schedule to attend to. She must be attentive to all the labouring women, every thirty minutes, including listening to the heartbeats of the unborn babies using a plastic or wooden equipment called a Pinard fetoscope. This is the reality for a typical midwife in the country where maternal and newborn mortality rates have remained persistently high. The menacing deaths, however, shouldn’t remain high if the rapidly advancing technology and innovative tools are harnessed to improve the quality of healthcare in such settings.
Now take this example of another busy midwife in similar rural settings, but working in a facility where technology is driving healthcare provision. The lone-and-busy-midwife is attending to as many pregnant women. But in this case, the labour room is equipped with an electronic device that is continuously connected to a pregnant woman who is in labour, to monitor the progress of the unborn baby. And the tool gives an alarm when the unborn baby is not doing well. The midwife relies on the alarms to take appropriate action on time. In such a scenario, the risk of maternal or newborn death during the midwife’s shift should obviously be lower compared to the scenario in a facility devoid of the tools to monitor patients.
Given the grim statistics about maternal and newborn deaths, there is a compelling reason to invest in such tools; in our endeavours to cut down preventable deaths, especially in areas where healthcare providers are overwhelmed.
Dr. Salvatory Kalabamu, HKMU
Do we have practical examples? Yes. The story of a midwife whose services are driven by technology and innovative tools is one good example–and this is happening in Tanzania though the implementation of the Safer Birth Bundle of Care (SBBC)- the innovative clinical and training tools for improved labour care and newborn resuscitation that are integrated with new strategies for continuous quality improvement.
In five regions of Manyara, Mwanza, Tabora, Shinyanga, and Geita, the SBBC intervention is implemented under the quality improvement program, through a consortium led by Haydom Lutheran Hospital. The program, which started in 2021 receives support from Global Financing Facility.
It serves as an example of how innovative tools can indeed play a big role in helping Tanzania achieve its target of cutting down the stubbornly high maternal and newborn deaths rates to no more than 70 deaths per 100,000 live births and 12 deaths per 1,000 live births respectively, as per Sustainable Development Goals(SDGs).
In 2020, the World Health Organisation estimated that in Tanzania, out of 100,000 women, 238 die of pregnancy and birth-related complications which is also above the global figure of 223 deaths per 100,000 live births. It is evident that Tanzania is lagging behind in attaining SDGs in maternal and newborn health. If the trend remains the same, the commitment to “leave no one behind” towards the 2030 agenda may not be realized.
How can SBBC help in tackling the challenge?
The technological innovations used in SBBC intervention clearly explains how this could work. This program entails using innovative teaching tools for enhancing health providers’ skills and competency in management of the most common maternal and newborn complications. Also, the innovative clinical tools are used for continuous monitoring of labour and effective manual ventilation of the baby who has failed to establish breathing on her own after birth (giving a baby air using a bag). The training is coupled with mentorship on how to use health facility data for continuous quality improvement. Such tools include:
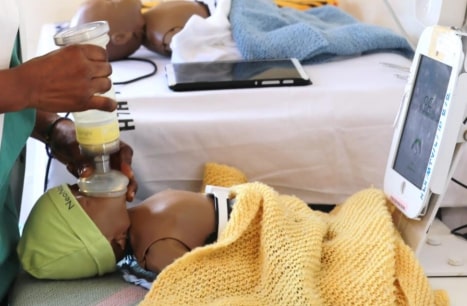
NeoNatalie live: Usually if any skill is not frequently used, it is gradually lost. This is also the case for healthcare providers’ skills and competency. Providers need to continuously enhance and consolidate their skills through practice. In SBBC intervention, NeoNatalie lives─ a “smart” dummy uses the internet connected to the tablet which displays feedback to trainees on their skills performance on how to give air to newborn babies who fail to breathe at birth. This ensures that they are always ready to help a baby who does not establish breathing after birth.
Neobeat: It is always difficult for a provider to differentiate a child who is born dead (called fresh still birth), and the one who is alive but too weak in such a way that he is not breathing, and his heart beats are too weak to detect using conventional means.

In SBBC intervention, Neobeat─ newborn heart rate meter which uses highly sensitive electro cardio-graphic technology is connected to the chest of a newborn to detect if the newborn is alive and to guide health providers to help the newborn to breathe. This aids the provider to provide to ventilate the baby continuously instead of pausing to count the heart rate which may delay hi p the child to breath on her own.
MOYO:
These are Foetal Heart Rate Monitors. This is where the story of the lone midwife I hinted at the beginning of this piece fits. MOYO is the electronic device that is continuously or intermittently connected to a mother who is in labor to monitor the progress of the unborn child.
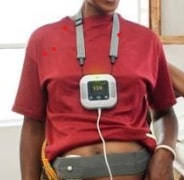
It gives an alarm when the unborn child is not doing well; this helps the healthcare provider especially in an overwhelmed labour ward to take appropriate action on time.
What has SBBC achieved?
Even though the intervention is ongoing, the interim analysis results on the ultimate outcomes are promising. During the annual SBBC stakeholders meeting at Haydom Lutheran Hospital on 23rd March 2023 the Principal Investigator of the project Dr. Benjamin Kamala highlighted the successes of the project in reducing maternal and newborn deaths. Notwithstanding that now the cost of per life saved cannot be realized, it is obvious that the intervention has gained tangible success.
What are the lessons learned?
There are several important lessons learned from this intervention; embracing technological and methodological innovations can enhance reduction in mothers and newborns deaths, and spin the wheels towards 2030 SDGs on maternal and newborn deaths. During routine deaths review, the “blame and shame” culture should be avoided to facilitate real data sharing and use the actual data to plan for continuous quality improvement strategies. In addition, stakeholders’ involvement, regular facility mentorship and supportive supervision are key for successful health intervention of this kind.